Forget the so-called breastfeeding mommy wars.
The big issue isn’t whether well-educated, middle-class moms choose to breastfeed their babies. The real problem—and one we should be talking fiercely about—is breastfeeding inequality.
Socioeconomic forces are drastically affecting breastfeeding rates in the U.S., and globally. The result: A huge number of mothers are not getting an equal opportunity to breastfeed their babies.
The stats may shock you.
Why It’s a Problem
- Socioeconomically disadvantaged moms are far less likely to breastfeed (or meet the American Academy of Pediatrics’ recommendations for optimal breastfeeding).
- Babies born into conditions of hardship tend to receive less adequate health care, parental involvement and nutritious supplementary solid food once weaning begins.
- Essentially, the health benefits of breastfeeding are even more important for less-well-off mothers and their babies, and yet far fewer are breastfeeding.
- This inequality is a shocking reality that must be tackled.
Let’s dig into the data to see the extent of the problem.
The Zip code lottery. State to state, breastfeeding rates vary enormously. Mothers living in richer states, like California, are far more likely to breastfeed than those in poorer states, such as Louisiana. Breastfeeding rates are correlated with family income and local hospital practices, among other factors.
With regards to hospitals, 24 percent of babies born in the U.S. are born in Baby-Friendly designated facilities. The Baby-Friendly designation is awarded to hospitals that meet the Ten Steps to Successful Breastfeeding guidelines. These are a set of practices and procedure such as educating families to make informed decisions about infant feeding and offering expert lactation support throughout and beyond the hospital stay.
Currently, 1 in 6 hospitals or birthing centers in the U.S. is Baby-Friendly designated. These are disproportionately represented in wealthier states where there is more money available to implement the initiative.
Education. The higher her level of education, the more likely a mother is to breastfeed her child. Only 36 percent of mothers whose education level is high school exclusively breastfeed their babies for the first three months. In contrast, 56 percent of mothers with an advanced degree do so.
Earnings. Just 38 percent of mothers living below the poverty threshold will breastfeed their baby until 6 months, whereas 68 percent of mothers from wealthy families (earning six times over the threshold) will do so.
That is a huge disparity, which is made all the more stark when you consider that in 2016 there were 40.6 million people in poverty in the U.S. That’s a lot of babies not breastfed, simply because of the socioeconomic conditions they were born into.
Some reasons that well-off mothers have improved breastfeeding rates are:
- Longer maternity leaves;
- Jobs that allow for pumping breaks;
- Better support networks;
- Better hospital practices;
- Ability to hire outside help;
- A culture that unconsciously views breastfeeding as a desirable status symbol.
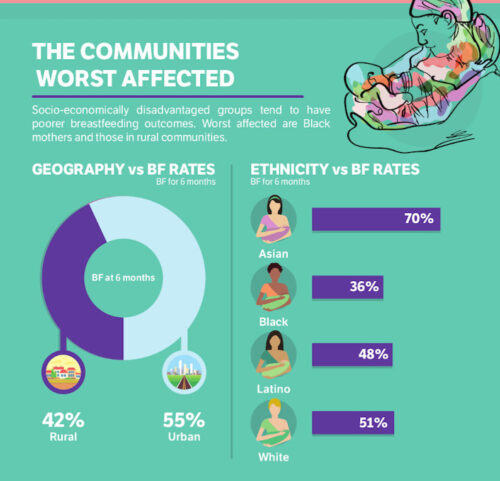
Urban/rural divide. Mothers in rural communities are less likely to initiate breastfeeding (42 percent of rural mothers will breastfeed to 6 months as opposed to 55 percent of urban mothers).
Studies indicated that rather than being caused by some inherent urban or rural culture, it has far more to do with confounding factors, such as maternal ethnicity and poverty level. Mothers living in rural communities are more likely to have a lower income and work in a job that doesn’t allow as maternity leave and doesn’t provide a lactation programme. They are also less likely to receive social breastfeeding support.
Ethnicity. There are significant disparities in breastfeeding rates among Asian, Black, Hispanic and White mothers. A major part of this trend has to do with socioeconomic measures such as poverty, education and relationship status.
Reasons for the difference, however, run deeper than income. Other influencing factors include whether a mother receives supplementary breastmilk in hospital, whether she has experienced a close family member breastfeeding and whether she believes breast is best.
One startling statistic is that Black mothers are nine times more likely to be given formula in the hospital than White mothers.
Another interesting insight is that Hispanic mothers from low-income families are more likely to breastfeed than their Black or White counterparts. The reasons appear to be that Hispanic mothers tend to experience another family member breastfeeding. This intergenerational influence plays a huge role in whether a mother chooses and successfully breastfeeds.
Formula use in the hospital. Breastfeeding rates differ from hospital to hospital. It is in part a worrying reflection on the differing quality of maternity and lactation support. (The silver lining is that this area may be one of the easier wins in the fight to reduce inequality.)
Use of formula within hospitals is an issue. Firstly, 66 percent of hospitals reported giving breastfeeding mothers free infant formula in their hospital discharge packs. Hospitals generally do this as part of an agreement with commercial formula brands in return for free formula provision.
Perhaps even more worrying is that 24 percent of maternity services provide supplements of commercial infant formula as a general practice within the first 48 hours after birth.
Both practices have been shown to negatively affects whether a mother exclusivity breastfeeds and for how long she does so.
Lactation support in the workplace. In the U.S., only 28 percent of workplaces are lactation friendly (i.e., provide comfortable and private rooms where mothers can use breast pumps and store milk safely). These tend to be in middle to high-income jobs. This is bad news for the majority of working mothers and creates another dimension of inequality. Especially since 25 percent more women breastfeed to six months if their workplace provides decent lactation rooms and breaks to express.
Clearly, there is a long way to go before mothers are properly supported in their breastfeeding efforts within their workplace. This is having a significant impact on the number of babies getting breastfed across the U.S.
Marital status. Married women are more than twice as likely to breastfeed for six months than mothers who have never married. Clearly, the support fathers can bring plays a significant role. New Zealand researchers found when dads cooked dinner (and washed up), it had a positive effect on the mother’s breastfeeding success. It allowed Mom time to focus on feeding the baby and provided her with rest that helped with maintaining her milk supply.
How to Reduce Breastfeeding Inequality
Too few mothers follow the AAP’s optimal breastfeeding recommendations. Were this a result of well-educated, well-informed and well-off women choosing alternative nutrition options, that would be one thing. Unfortunately, the truth is that many babies are formula fed because their mothers are not sufficiently aware of the health risks or they simply don’t have practical support (at work or home) to make it work.
This is unfair and impacts on the health of thousands of U.S. mothers and babies each year. It has been estimated that annual excess deaths attributable to suboptimal breastfeeding total 3,340, 78 percent (2605) maternal and 22 percent (735) infant.
But how can we reduce breastfeeding inequality?
While there is no easy fix, there are several strategies that have been highlighted and could use public awareness and support. These are:
- Maternity/lactation support – Improve hospital maternity care and lactation support practices. For example, increasing the number of Baby-Friendly Designated hospitals across the U.S., especially in states with more poverty;
- Educate professionals – Continued education of health care professionals such as doctors, nurses, midwives and lactation consultants, to improve their knowledge, skills, attitudes and behaviors toward breastfeeding support;
- Improve new mother access to professional lactation support – This can be done in different ways, such as in-person, online, telephone or group. It can involve home visits or breastfeeding clinics within the community;
- Peer support programs – Peer support is a powerful mechanism for helping mothers reach their breastfeeding goals. Effective peer support typically requires leaders to be trained as facilitators. Mothers then share emotional support as well as guidance and problem-solving advice, e.g., tips for getting a good latch or breastfeeding in public;
- Boost breastfeeding support in the workplace – There are numerous ways in which employers can support mothers to continue breastfeeding. These include developing corporate policies, and providing adequate lactation spaces and equipment and giving women the flexibility to use them. Onsite childcare and allowing babies at the workplace also helps;
- Support for breastfeeding in childcare and pre-kindergarten settings – Many mothers have older siblings attending early care education centers (e.g., Head Start or pre-K). This solution involves improving the support that these centers give to breastfeeding mothers, e.g., welcoming breastfeeding mothers to come into the center or training staff to handle the storage and use of pumped breastmilk;
- Improved access to breastfeeding education and information – While many mothers have heard the message that “breast is best,” many new mothers do not have direct experience of breastfeeding. It is vital that breastfeeding education and information get into all communities, especially minority groups that can be harder to reach;
- Address the marketing of infant formula the associated conflict of interest in hospitals – There exist well-established links between commercial formula companies and hospitals. In return for free infant formula for babies that need it, many hospitals agree to give away free formula within their discharge bags. There is also a high incidence of hospital routinely supplementing breastfed infants with formula within the first 48-hours. Both of these practices lead to an increased uptake in formula use and a corresponding drop in breastfeeding rates. It is important that marketing practices that directly reduce breastfeeding rates are dismantled and replaced with others that do not involve a conflict of interest.
Equality of Knowledge and Breastfeeding Opportunity
The breastfeeding mommy war is a huge distraction from the real problem of inequality. If a well-informed mother makes a carefully considered decision not to breastfeed, that is entirely up to her. This isn’t the issue. The real issue is that not all mothers have equal knowledge or opportunity when it comes to making the right breastfeeding choice for them and their baby.
If breastfeeding inequality is tackled, then hundreds and thousands of more babies will be breastfed. This, in turn, will lead to improved health outcomes for mothers and babies and economic benefits to society.
Let’s shift the focus of the conversation to breastfeeding inequality. It’s here that the biggest wins in health and well-being outcomes can be made.
—Neve Spicer
From We the Parents.